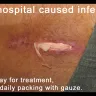
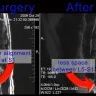
unethical behavior from a insurance business - not answering or returning call on a automobile accident case.
My lawyer has been trying to resolve my car accident case since September 2016: Claim Number: [protected]-0001.
The Claims Adjuster does not answer their telephone calls or return the calls to the Adjuster on the Case. This has been happening since September of last year .
I believe Sedgewick Insurance Company is a very unprofessional company for not answering clients questions; I do not know how they are still in business for Insurance purposes.
I would like a expedient answer to my lawyer on their phone calls so I can have this case settled with a great offers as soon as expediently possible. Lawyers are Saiontz and Kirk - 3 S Frederick Street - Suite 900; Baltimore, Maryland [protected] or [protected] or [protected].
This is uncalled for; just going back and forth with leaving messages and no answer!
manhattan sofa and chaise
In April of 2016, I had my sofa and chaise repaired by one of you're repair men you send out. The spots repaired look really bad. Discoloration and peeling where it was repaired. Iam very unhappy about it. Last week, I filed a claim with Sedgwick. Today I hear from an Adjuster regarding my sofa nor chaise are either covered on the BCP. I purchased the 2 year agreement. The adjuster stated you all can send out another repair man to fix it again. No that will not work. I do not need another repair man to ruin my sofa and chaise again trying to repair it. I want it replaced. It is not my problem you all used faux (fake) leather. I will contact the BBB regarding this issue if this is not resolved.
Deon Carter is the adjuster handling my claims. The claim #'s are [protected] and [protected]. Contact me regarding this issue. I'm sure your company can eat the measly $800 we paid for this sectional set so we can have a nice sectional worth our money. Please email me for photos as I was unable to upload them.
Thanks,
Kelly Kendrick
claim service
After a month of trying to reach this company I finally got paired with a claim examiner. After 3 months of trying to get everything in order with the company I finally was able to get a rental and put my car in the shop. The shop still has multiple days of work left to do on the car, but enterprise (The car rental company) has not been able to reach the company regarding the rental. I have tried to reach out to my examiner every day from 01/09-01/12 with no avail. Now I can't even reach anyone from the company at all and I have been hung up on twice. I really need assistance in regards to this situation.
housing claim submitted
The worst claim company ever. I would not recommended selecting them. Here's why: i've had a claim submitted with sedgwick for over a month now and i'm still chasing a ghost for an answer. My claim specialist was a man named steven fryer. This rep never answers his calls, never responds to emails, ignores your calls for even an update and sends you straight to his voice mail that he probably just erases. If this is just one service rep, the others are probably the same. So incompetent!
After a month of me having to comply with images of damages, me constantly emailing, having their reps exhibit several inspections of the horrible floor damages; admitting to them making the damages, he then denies my claim does not return a call or email but sends a letter of denial saying there was not enough proof. When you can clearly see the damages the clients made on my floor and it is still not fixed. Very unprofessional, if there were other actions I can take to let others know how bad their service is I will. Others who are thinking of going with them, refrain. They will have you going around and around in circles only to un-service you in return.
christopher collier claims rep
At Family Dollar on Central Street and Lynn Mass a shelf fell on top of my daughter when we was getting our Christmas tree when it fell we scream for help no employees came to help... I had to lift the shell off my daughter when I already have severe back pain that I am on monthly medicine for with ulcers we made a complaint 2 Family Dollar manager he went to the aisle to move shelf so no one else gets hurt... the employee apologize but my daughter still got hurt... Christopher collier reached out to me a month later, he then told me i never received health forms because they had no address for me, which i believe is not correct, they did have my address or how would he have received my phone number! So Christopher then tells me they have the security footage and the shelf indeeds falls on my daughter and if i have health insurance they have to cover my daughter injuries... And that she will receive a 1, 000 check for an award...and i need to have the health forms back to him asap... Then today i call about some questions and he pretends we never had a conversation, i have two witnesses from work when Christopher called me that day about the health forms and the check, because he was on speaker phone because i was at work, today he states he never called two weeks ago and that he didnt offer nothing to my daughter and he was very rude... When he called two weeks ago and was talking about the security footage and explain everything down to detail, now he acting like we never spoke... I want something to be done now about this... Thank you and happy new year!
file a complaint with the INSURANCE COMMISSION
prescriptions
My name is michele haywood. I have been under a worker's comp claim since august 14, 2013.
Since august, 2016, I have been having extremely long wait times for any or all three of my prescriptions to be filled by the pharmacy - publix in merchant's crossing, englewood, fl for the hydrocodone (Because they always have it, without fail) and the walgreens @ oriele in englewood, fl for the nabumetone and tizanidine.
My former claims adjuster, hunter shaw, left without a warning, I believe the current one is lori buck whom I never hear from.
One of these medications has nasty side effects when not taken properly; and another medication prevents spasticity.
Why does it take so long to approve them? And, how can I get them approved the day I turn them in—when they are due?
This is my second or third complaint on approval services.
Thank you,
Michele haywood
6190 marcum street
Englewood, fl 34224
[protected]
std
This company has caused me nothing but stress and complications. My claim Was originally approved for the Exact time frame my doctor recommended weeks later the examiner calls and tell me they approved it for a week shorter, At this time I haven't even had a follow up after my surgery. This company do not care about your situation or finances, I sent in the required paperwork from my doctor to get the remainder of my week and till this day no one has reviewed it this is unprofessional and just goes to show how much they care. this company needs to be Shut down and never gain business again.
std
Ive been on std for about a month. My account manager michael tierney never responded to my calls or emails days approaching christmas... He called me 2 days after christmas informing me he was off for the holidays... While i'm here with 3 daughters and sedgwick managed to screw up my pay the week before christmas... So no pay and no explanation other than letting me know that he was off for the holidays. I think is a terrible shame that I have no other choice other than to deal with this incompetent company... I work for pepsi... And this is what I have to deal with. Thanks sedgewick...
workers compensation
Patient was injured on job and awarded workers compensation. However, patient is not being fully compensated for a 40 hour work week for several months now. Mileage to doctors appointments and physical therapy also take 3-4 months to be reimbursed for. Business is unable to provide adequate answers as to why patient is not be reimbursed correctly for pay and mileage reimbursement.
to be paid for my transportation and other things I paid for while under workmen compensation.
Hi, the company sedgwick cms does not respond to my emails below and it has been months.
Can you please let me know if you received my email and what is being done?
Thanks, dave
From: david hartwig
Sent: friday, october 28, 2016 4:03 pm
To: '[protected]@sedgwick.com'
Subject: information for david hartwig, claim# [protected]
Hi,
I cannot get any response from austin, please advise.
Thanks, dave hartwig.
Hi austin,
It is october 25, 2016 and I have not heard anything from you, please let me know what is going on?
Thanks, dave
From: david hartwig
Sent: tuesday, september 20, 2016 12:04 pm
To: 'austin. [protected]@sedgwick.com'
Subject: information for david hartwig, claim# [protected]
Hi austin,
I have attached information on my claim# [protected].
work injury claim
I was injured at my job 9/29/15 where they had me fill out paperwork regarding my injury site, that asks for information I could not possibly know minutes after it happened. So I did my best guess in order to open a claim and be able to see a doctor to be treated. They first suspected a rotator cuff injury, which over the course of a few months and several specialists determined it was a neck injury and my nerves are a damaged which was why the pain would also be in my shoulder. The IME they paid for determined I was physically perfect and okay. I contested it as I still experience immense pain and numbness and tingling, and cannot lift or support much weight at all on the injured side. They gave me a second IME which led to them permanently closing my claim. I'm 20 years old, was offered at one point, long term disability, have lost feeling in half my right hand, experience chronic neck pain, numbness and tingling in my shoulder/shoulder blade. All seemingly permanent. They denied me the right to seek further imaging, they denied me my right to get away from narcotic medications by being referee o a pain clinic, and then denied me my rights to any medications all together and closed the claim regardless of how hard I contested it and fought with them. If I was as physically perfect and healed as they said I was, then why am I still suffering every minute of everyday since?
rental car coverage
Hi I was a victim in a car accident 11-04-2011 the person driving was responsible for my injuries and the fraud I'd like to add new info to possibly reopen my claim and to seek criminal charges on this person he also has covertly ruined my life by placing me under a computer monitoring system so I would not be able to get any help pls contact me to tell me how to do this I am disabled and I have no car I have 2 conflicting police reports and wrong information is given by him of course as I was in the hospital for 9 days immediately after he also committed crimes on my kids and my baby was kidnapped as a result of this monitoring system in New Orleans again its long story I have nothing but time but I need someone to please contact me the investigator was D.Seymour in lvmpd my name is Cecily Higginbotham I was a passenger in a fully covered rental car and prevented from collecting claims due to fraud then more crimes were committed on me through this monitoring system technology [protected]
unethical behavior
DOI: 04/16/16
Claim #[protected]
Patient: Lynn Everitt
Contact at Treating Facility:
Sarah Detrick- [protected]
[protected]@aptclinics.com
This patient was evaluated at our facility, Advanced Physical Therapy, on 09/21/16 for a lesion in her ulnar nerve causing pain in her right wrist. The script from her physician requested she be seen 2-3 times per week for 6 weeks until her follow-up appointment with him on 10/20/16. However, the original authorization was only for 6 visits.
The patient's evaluation note and script were submitted to Medrisk for an additional 6 visits on 9/27/16.
On 10/4/16 the authorization request was resubmitted because we were told that the original had been misplaced.
Sedgwick CMS denied the proposed treatment plan from her referring physician, and only authorized 6 visits for the patient. After denying the authorization request no one informed the third-party claims company Medrisk of the denial, nor did they contact the physician, or treating facility.
On 10/17 we tried to contact the patient's adjuster from Sedgwick CMS, Arielle Richards, but her voicemail stated that she was gone on vacation and to contact her supervisor instead.
We contacted her supervisor, Brandi, who informed us that the issue with the authorization request, according to the Utilization Review nurse's notes, was that the script wasn't "Up-to-date". I informed her that we also had a signed plan of care approval from the referring physician that should also act as an additional more "up-to-date" script, but she wasn't certain what I should do with it. She forwarded me to the UR nurse, Dana, who informed me that a plan of care request isn't a script, even though it is signed by the doctor, would "possibly not be approved", if submitted with an authorization request.
Submitted new authorization request to UR, the case manager, and Medrisk on 10/20 with plan of care signed by the physician for an additional 8-12 visits.
Patient had a follow-up with her referring physician on 10/20/16 where he wrote a new prescription for an additional 18 visits.
Submitted new authorization request on 10/26/16 as well as contacted Brandi, the adjuster supervisor, to see if there had been any updates at all on this matter. She informed us that all of the previous authorization requests had been denied because the UR nurse had labeled them all as "duplicates". Left a message for the UR nurse to call us back to resolve the issue.
Dana, the UR nurse called back on 10/28/16 to let us know that the newest authorization request had been denied due to them not being able to talk to the referring physician for a peer-to-peer review.
We then called Dr. Gwyn, the referring physician, whose nurse informed us that he had tried to call Dana back several times but was never able to get a hold of her.
Resolution: This patient is, and has been in a considerable amount of pain since the DOI, and would greatly benefit from therapy according to her referring physician and our occupational therapist who is treating her. We are asking that her physician's scripts be honored, and ultimately be authorized for her 10 current visits to be covered, as well as the additional 20 visits requested by her physician. Please feel free to contact Sarah in referrals with any questions or if any additional information is needed.
failure of filing short term disability
I was diagnosed on September 14, 2016 with what has turned out to be a severe case of Bells Palsy. Since driving and work period requires using your eyes, and in my line of work I deal with chemicals, dirt, forced air, I work in a hospital, I was removed from my job and told to file short term disability. It has been the biggest nightmare of my life. I have blurred vision, double vision and am unable to close my affected eye. I cannot wear a patch due to the fact it does not form a seal around eye allowing air and dir to get in. I cannot keep my eye taped shut due to the skin breaking down and blistering and causing sores. I have letters from my eye Dr and my ENT who specializes in severe case of long term Bell's palsy stating that I am unable to work or drive at this time. Sedgwick has still denied my claim. I am appealing it for the second time and will probably loose my home and car before this is settled. Every time I speak to someone at their office they don't seem to know what the other claims adjuster or rep has said, they are unable to find faxes that I have had sent and are very condescending and the way they talk to me. They are the most dishonest company I have ever seen or dealt with and definitely have no empathy or sympathy for their customers and I am a paying customer as I pay monthly to have disability through my job
broken faucet and pipe damage occurring on 8/24/2016 by sears repairman
On 8/23/2016 a Sears repairman while working on my lawn mower ran over and broke a yard faucet, to the point of bursting the galvanized pipe going to faucet in both directions, on main line to house. Repairman advised me to get a plumber to repair faucet then send Sedgwick the bill and they would repay me. I did get faucet repaired, sent bill to Sedgwick and was contacted by an adjuster, Matthew Greenlee. He informed me to send an itemized bill, which I have done twice. Since Mr Greenlee called me I have not been able to reach him by phone, this going on the second week now. I would like to get this resolved as soon as possible by getting paid what the insurance company will pay me. My name is Bobby Johnson. The claim number is L1608245107-0001. Thank you for your attention in this matter.
sedgwick auto claim
My husband was rear ended by a rented Budget Truck on 7/8/16. The guy driving the truck didn't have insurance and Budget didn't make him purchase insurance. I was directed to Sedgwick because they handle the claims for Budget and Avis. First of all, it took them 2 weeks to even admit that they would be responsible for this. They kept telling me to contact my own insurance company--pay the deductible and go that route. I would not as I did not want my insurance to go up because of this. Finally they accepted responsibility but kept refusing to pay for a rental while our truck was in the shop. After many phone calls which just went to voice mail and literally 50 emails which also went unanswered, I was finally able to reach a supervisor and after telling him I'd spoken to an attorney--he finally agreed to get us a rental. At one point during the repair, they did not extend the rental like they should have and when trying to reach ANY of the claims agents--was told they were all out of the office for over a week. Avis had started taking money out of my bank account and was threatening to turn me in for stealing the car if I didn't return it. After an entire day of calling and emailing, I finally got someone to extend the rental. The body shop turned in supplements to the repair estimate and it took Sedgwick over a month to ok the repairs. Our truck was in the body shop for over 2 and a half months on a repair that should have taken a week or 2--only because they took forever to give the go ahead on things.
My husband also got whiplash in the accident as he was at a stop light and the guy just ran into him--TWICE--I had to locate and pay a doctor myself. They said they'd cut a check for the doctor bills when it was all over as well as compensate us for pain and suffering. My husband missed numerous days of work because at his job he can't just miss a few hours for a dr appt--it is shift work. He had to see the doctor and Chiropractor for 3 months. He was finally released the beginning of October. Here it is the 26th of October and we are still dealing with this. They offered a settlement that would cover the Chiropractor and not much over that. Not accounting for lost wages and such. I am going to call my lawyer and see if there is anything that can be done with out having to spend years in court over this.
These ppl have been nothing but rude and uncooperative from the beginning. They NEVER answer the phone or return messages or emails. I honestly don't see how they are still in business. If we are ever in a situation where we have to deal with them again--I won't--I'll just turn the entire thing over to a lawyer and let him deal with it.
medical injury claim
I had a spine surgery conducted at ucla. The surgeon neglected to install the intervertebral body cage that was supposed to be part of my operation. Without that device, my surgery failed and sedgwick instantly decided that I didn't have a claim.
I don't believe that doctors should be able to lie to their patients about the details of their surgical procedure and get away with no punishment. Sedgwick doesn't care about patients or truth or fairness. They just want to save their client money any way they can. They are a criminal organization that colludes with corporations to screw their victims out of settlements.
samuel saldivar claims dept
I have never dealt with such a rude, uncaring, sarcastic, lazy, lying unprofessional individual! I was assigned to this man since the end if June. My car has been in the shop for 2 months! Samuel Saldivar said and ok'd to the repairs but has yet to finalize everything. I am calling daily, leaving messages.. He does not respond or says he's doing something yet does nothing..he keeps requesting ridiculous things from me and I comply and then he asks for something else! I find him abusive and especially since ne husband passed away and I'm dealing with death and he just doesn't give a dam. I think it's his thing to upset and belittle women and with this job he gets away with it! I am forced to hire an attorney as I am going to have a breakdown. Nervous breakdown that is and he is just not worth it! He is despicable and yes I am posting on every social media and have skso spoken to the TV station and my story will be aired soon!
short term disability
My husband was diagnosed with epilepsy 2 years ago. He recently began having seizures through the medication so his doctor suggested going on short term disability to undergo testing to get to the root of the problem. STD began July 5, 2016. The doctor ordered a lot of testing and ultimately referred us to an epilepsy lab in Houston, TX (4 hours from home...
Read full complaint and 4 commentsworkers compensation
A large box of 27 FULL 39-lb freon tanks opened up in the rear of my van and were rolling around. I pulled over on the highway and two of them rolled out onto the highway. When I went to pick them up, I heard/felt POP in my back. Now they're trying to say that it was pre-existing. Ridiculous.
I've done EXACTLY what they've instructed. Went to THEIR doctors who have all written that I'm not allowed to work but now @Sedgwick wants a second opinion -OF THEIR OWN DOCTOR -and is trying to say it's not work related even though the orthopedist clearly wrote "degenerative changes with inflammation and pain related to injury".
So, I can't go to work because the doctor wrote me out, but I can't afford to stay out of work. Ridiculous.
It can not be legal (and is certainly not ethical) to be told that you cannot go into your office because a doctor said you can't but also are not going to be paid for that time!
I have already filed complaints everywhere I can think. Any suggestions are welcomed. I absolutely plan to sue.
A large box of 27 FULL 39-lb freon tanks opened up in the rear of my van and were rolling around. I pulled over on the highway and two of them rolled out onto the highway. When I went to pick them up, I heard/felt POP in my back. Now they're trying to say that it was pre-existing. Ridiculous.
I've done EXACTLY what they've instructed. Went to THEIR doctors who have all written that I'm not allowed to work but now @Sedgwick wants a second opinion -OF THEIR OWN DOCTOR -and is trying to say it's not work related even though the orthopedist clearly wrote "degenerative changes with inflammation and pain related to injury".
So, I can't go to work because the doctor wrote me out, but I can't afford to stay out of work. Ridiculous.
It can not be legal (and is certainly not ethical) to be told that you cannot go into your office because a doctor said you can't but also are not going to be paid for that time!
I have already filed complaints everywhere I can think. Any suggestions are welcomed. I absolutely plan to sue.
Bankrupting our family over legit claims with multiple doctors and surgeons testifying as to my husband’s need for hip surgery. Absolutely the worst company and disgusting how terrible they treat people. They should be sued for malpractice! As if being unable to work and being in severe pain isn’t bad enough they make a very simple process horribly complicated and delay basic medical care! How are they getting away with this?!?!?! #classactionagainstsedgwick
Get a lawyer! Do not listen to anyone who says you do not have a claim. I'm interested in the know-it-all who comments "How did you get injured by bending over to pick up something?" This is not rocket science, but it definitely is pre-judging someone who is simply replaying what happened. A person transporting equipment behaves in a safe manner, pulling the truck to the side of the road, works quickly to get their tanks out of the middle of the road. Are they focused on good body mechanics? or getting the stuff out of harm's way? And what does it matter anyway? Workman's comp is in place to cover accidents. You figure the person planned this scenario? Give yourself a an A+ at being a jerk.
I can see their point actually. How did you get injured by bending over to pick up something? It sounds as though you did not practice safe lifting.
About Sedgwick Claims Management Services